Dr. Mario Nicolosi Specialista in Ortopedia e Traumatologia Specialista in Fisiatria
Reconstruction of the glenohumeral ligaments in anterior and anterior-inferior recurrent dislocation of the shoulder
For recurring anterior and anterior-inferior shoulder
dislocation, we have carried out the Neer and Latarjet
operations for years with great satisfaction. Although we have
been pleased with these two methods, we are always on the
look-out for an operation which is even more physiological and
effective.
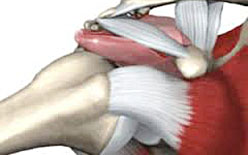
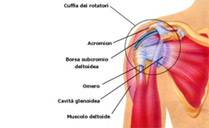
Our intention was to restore the previous anatomical state as
much as possible, reconstructing the anterior glenohumeral
ligament and putting the inferior glenohumeral ligament under
tension without shortening the capsule, translating or osteotomy.
In order to reach this goal, we proceed as follows.
The subscapular is reached via the classic Larghi incision and
is then sectioned away from the capsule. Here, an oblique
arthrotomy is performed from the top to the bottom and from the
inside to the outside, following the middle glenohumeral
ligament. Once the humeral neck has been reached, the capsule is
completely detached at the insertion of the inferior
glenohumeral ligament so as to be better able to mobilize the
capsule during the reconstruction. After completion of the
arthrotomy the articulation is explored in search of possible
Bankart lesions which, if present, are repaired. After this, the
capsule is sutured. The syndesmoplasty is performed by
overlapping the two capsule halves, suturing the medial half a
bit laterally but mostly shifted in an upward direction.
This kind of sutured shift doubles, and therefore reinforces,
the middle glenohumeral ligament and puts the inferior
glenohumeral ligament under tension. A further advantage of this
sutured shift is that the capsule is not shortened and thus does
not reduce extrarotation. After completion of the syndesmoplasty
it is possible to greatly extrarotate the shoulder. To finish,
the subscapular is sutured back into place. This is followed up
with four weeks of shoulder immobilization, followed by
kinesitherapy.
From 1993 to 1996 we operated on 34 patients. Of these, 31 were
men and 3 were women. The average age was 21 years old. The
average follow-up took place after three years.
The results were very satisfactory: excellent in 76.6 %, good in
17 .6 %, sufficient in 2.9 % and bad in 2.9 %. The first case
operated on continued to have a subjective feeling of
instability, however without episodes of dislocation; in the
other 33 cases we had no further dislocations and all the
patients returned to their previous work and sports activities.
We would like to point out the advantages this method offers:
the simplicity of the surgical technique, respect for the
anatomy, the speed of and complete return to shoulder mobility.
1) It is simple because we are only dealing with a normal
arthrotomy and a normal overlapping suture. Furthermore, if
there are no associated lesions in the glenoid labrum to be
repaired with screws or anchors, the technique requires leaving
no foreign objects in the site.
2) It respects the anatomy because it does not require osteotomy
or complex transpositions and because it returns the anterior
and anterior-inferior portion of the capsule to its normal
physiology.
3) It brings about fast and complete return of shoulder mobility
because this kind of syndesmoplasty does not shorten the capsule
and, therefore, does not result in reduced movement.

 Laureato in Medicina e Chirurgia presso l'Università di Catania,
specializzato in Ortopedia e Traumatologia presso l'Università di Bologna
(Istituto Rizzoli) e specializzato in Fisiatria presso l'Università di Trieste.
Laureato in Medicina e Chirurgia presso l'Università di Catania,
specializzato in Ortopedia e Traumatologia presso l'Università di Bologna
(Istituto Rizzoli) e specializzato in Fisiatria presso l'Università di Trieste.